We’ve all gotten sick or scraped our knee. It’s part of being human. It’s why we all know how uncomfortable it can be when a scrape starts to swell or our joints start to ache when we’re sick. Well, what causes that reaction precisely? Inflammation.
And if you’ve ever been sick, injured or are just getting older, you likely know how much joint inflammation can impact our daily lives. Given the complexity of the subject, the Baxyl® Team thought the webizens that frequent our blog might enjoy a deep dive into all things joint inflammation. So, let’s discuss...

What is Inflammation?
Inflammation and swelling are often terms that are used interchangeably. When we are sick or injured, our body’s immune system sends out a response to attack the invading pathogens or heal damaged tissue. This is called an inflammatory response. It is the body’s normal immune response to an injury, infection or other irritants. And, it’s all the excess blood and cells being diverted to help your deal with a pathogen or injury that causes swelling assosciated with inflammation.
It’s important to know that there are different types of inflammation. Inflammation can be either acute or chronic. Acute inflammation is the body’s immediate or short-term response to infection or injury, while chronic inflammation may last months or even years.
Allergies, wounds and diseases can all cause inflammation. The most common causes of joint inflammation are injuries and inflammatory arthritis.
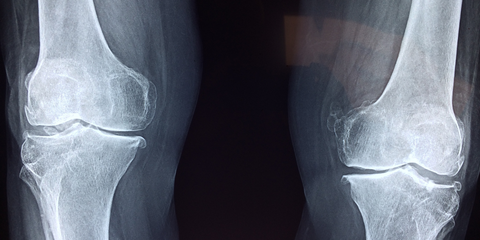
What Is Joint Inflammation?
Joint inflammation, known medically as arthritis, encompasses a range of conditions characterized by inflammation and pain in the joints.
Several factors can contribute to joint inflammation. As leaders in the joint supplement marketplace, the makers of Baxyl® want to provide you with a complete guide of what causes joint inflammation, how to treat that inflammation and some ways that may prevent it from happening.
8 Factors that Cause Joint Inflammation
1. Autoimmune Disorders
Autoimmune disorders that lead to joint inflammation, also known as autoimmune arthritis, include several conditions where the immune system mistakenly attacks healthy tissues in the joints. This results in inflammation, pain, stiffness and joint damage.
Some of the common autoimmune disorders that can cause joint inflammation include:
Rheumatoid Arthritis (RA)
Rheumatoid arthritis (RA) is a chronic inflammatory autoimmune disease that primarily affects the synovium, or lining of the joints. In RA, the immune system attacks the synovial tissue, leading to inflammation, joint swelling, pain and eventual destruction of cartilage and bone. RA can affect multiple joints symmetrically and may also impact other organs and systems in the body.
Systemic Lupus Erythematosus (SLE)
Systemic lupus erythematosus (SLE) is a systemic autoimmune disease that can affect various organs and tissues, including the joints. Lupus-related joint inflammation can cause arthritis, stiffness and swelling, particularly in the small joints of the hands, wrists and knees. Joint symptoms in SLE may fluctuate and often occur alongside other systemic manifestations such as skin rashes, fatigue and organ function.
Ankylosing Spondylitis (AS)
Ankylosing spondylitis (AS) is a chronic inflammatory arthritis primarily affecting the spine and sacroiliac joints, leading to stiffness, pain, and eventual fusion of the spine. AS can also affect other joints such as the hips, shoulders and knees, causing inflammation and reduced mobility. It is characterized by inflammation of the entheses, the sites where ligaments and tendons attach to bone.
Psoriatic Arthritis (PsA)
Psoriatic arthritis (PsA) is a form of inflammatory arthritis that occurs in some individuals with psoriasis, a chronic autoimmune skin condition. PsA can affect the joints, skin, nails and entheses, causing joint pain, swelling, stiffness and psoriatic skin lesions. Psoriatic arthritis can affect any joint, including the small joints of the fingers and toes and may also involve the spine (spondylitis).
Juvenile Idiopathic Arthritis (JIA)
Juvenile idiopathic arthritis (JIA) refers to a group of chronic inflammatory joint conditions that affect children under the age of 16. JIA includes several subtypes characterized by persistent joint inflammation, pain and stiffness, which can lead to joint damage and disability if left untreated. The exact cause of JIA is unknown, but it is believed to involve autoimmune mechanisms.
These autoimmune disorders require careful management by healthcare professionals, including rheumatologists, who specialize in diagnosing and treating autoimmune arthritis. Early diagnosis and intervention are crucial for improving outcomes and quality of life in individuals with autoimmune arthritis.

2. Infection
Bacterial, viral or fungal infections can trigger joint inflammation. Bacterial infections such as Lyme Disease can cause infectious arthritis, while viral infections like hepatitis B or C can lead to viral arthritis.
Infections can cause joint inflammation, a condition known as infectious arthritis or septic arthritis. Here's how infections lead to joint inflammation:
Direct Invasion
Infections can directly invade the joints through various routes, including bloodstream dissemination, direct inoculation from trauma, surgery or extension from adjacent infected tissues. Bacteria, viruses, fungi or other pathogens can enter the joint space, triggering an inflammatory response.
Inflammatory Response
When pathogens enter the joint space, the body's immune system recognizes them as foreign invaders and mounts an immune response to eliminate the infection. Immune cells release inflammatory mediators such as cytokines, prostaglandins and leukotrienes that promote inflammation and recruit additional immune cells to the site of infection.
Synovial Membrane Involvement
The synovial membrane, also known as the lining of the joint capsule, becomes inflamed in response to the presence of pathogens and inflammatory mediators. Synovitis is the inflammation of the synovium and leads to increased production of synovial fluid and swelling within the joint cavity.
Cartilage & Joint Tissue Damage
Inflammatory processes within the joint can cause damage to articular cartilage, synovial tissue and other joint structures. Prolonged inflammation and tissue destruction can result in erosion of cartilage, bone loss and joint deformity if left untreated.
Clinical Symptoms
Infectious arthritis typically presents with acute onset of joint pain, swelling, warmth, redness and limited range of motion in the affected joint. The joint may be tender to touch, and individuals may experience systemic symptoms such as fever, chills, fatigue and malaise.
Microbial Pathogens
The specific microbial pathogens involved in infectious arthritis may vary depending on the source of infection. Bacterial pathogens such as Staphylococcus aureus, Streptococcus species and Neisseria gonorrhoeae are common causes of bacterial septic arthritis. Viruses such as hepatitis B and C, herpes simplex virus and parvovirus B19 can also cause viral arthritis. Fungal and mycobacterial infections are less common but can lead to fungal or mycobacterial arthritis.
Risk Factors
Certain factors increase the risk of developing infectious arthritis, including underlying joint disease, compromised immune function, joint surgery or trauma, intravenous drug use, the presence of prosthetic joints and preexisting medical conditions such as diabetes, rheumatoid arthritis or systemic lupus erythematosus.
Early recognition of symptoms and appropriate management can help minimize joint damage and improve outcomes in individuals with infectious arthritis.
3. Injury or Trauma
Acute injuries, such as fractures, sprains or ligament tears as well as chronic overuse injuries can lead to inflammation in the affected joints. Repetitive stress or trauma can damage joint structures and trigger an inflammatory response.
Joint inflammation can also result from acute injuries, repetitive stress or chronic overuse, leading to conditions like traumatic arthritis or post-traumatic arthritis. Injuries to the joint structures, including ligaments, tendons, cartilage and bones, can disrupt normal joint function and trigger an inflammatory response.
Acute Injuries
Acute injuries such as fractures, dislocations, sprains and ligament tears can cause immediate swelling and pain. The inflammatory response helps initiate tissue repair and healing but can also contribute to tissue damage and joint dysfunction if left unchecked.
Chronic Overuse
Repetitive stress or overuse of the joints is common in athletes, manual laborers and individuals with certain occupations or hobbies. Repetitive stress on the joints can lead to chronic inflammation and degenerative changes in joint tissues. Conditions like osteoarthritis and tendinitis may develop over time, resulting in persistent joint pain, stiffness and functional impairment.

4. Metabolic Disorders
Several metabolic disorders can contribute to joint inflammation, leading to arthritis or arthritic-like symptoms. Some of the metabolic disorders associated with inflammation include:
Gout
Gout is a type of inflammatory arthritis caused by the accumulation of uric acid crystals in the joints. Elevated levels of uric acid in the blood, known as hyperuricemia, can lead to the formation of urate crystals in the joints, particularly the big toe, ankles, knees, wrists and elbows. The deposition of urate crystals triggers an inflammatory response, resulting in sudden and severe joint pain, swelling, redness and warmth. Gout is often associated with dietary factors, genetics, obesity and certain medications.
Pseudogout
Pseudogout, also known as calcium pyrophosphate deposition (CPPD) disease, is another type of crystal-induced arthritis characterized by the deposition of calcium pyrophosphate crystals in the joints. Pseudogout typically affects the knees, wrists, ankles and shoulders and can cause acute episodes of joint inflammation, pain and swelling resembling gout attacks.
Hyperparathyroidism
Hyperparathyroidism is a condition characterized by overactivity of the parathyroid glands, leading to elevated levels of parathyroid hormone (PTH) and disturbances in calcium metabolism. Simply put, the PTH plays a role in regulating the body's blood level of calcium and phosphorus. Chronic hyperparathyroidism can cause calcium deposition in soft tissues and joints, contributing to joint inflammation and pain.
Wilson’s Disease
Wilson’s disease is a rare inherited disorder characterized by abnormal copper metabolism and accumulation of copper in various organs, including the liver, brain and joints. Joint involvement in Wilson’s disease can manifest as arthritis, particularly affecting the knees, wrists and ankles.
Hemochromatosis
Hemochromatosis is an inherited disorder characterized by excessive absorption and accumulation of iron in the body’s tissues and organs.
Joint usage in hemochromatosis can lead to arthropathy, characterized by joint pain, stiffness and swelling. Iron deposition in the synovium and articular cartilage can contribute to joint inflammation and damage over time.
Ochronosis
Ochronosis is a metabolic disorder caused by the accumulation of homogentisic acid due to a deficiency of the enzyme homogentisate 1,2-dioxygenase. Ochronosis can lead to the deposition of homogentisic acid in the joints, cartilage and connective tissues, resulting in arthritis, joint pain and stiffness. Ochronosis is often associated with alkaptonuria, a rare inherited disorder of tyrosine metabolism.
Early diagnosis and appropriate management are essential for improving outcomes and quality of life in individuals with metabolic-related joint inflammation.
5. Inflammatory Bowel Disease (IBD)
Inflammatory bowel diseases, such as Crohn’s Disease and ulcerative colitis, are associated with joint inflammation and arthritis-like symptoms due to systemic inflammation and immune system dysfunction.
Inflammatory Bowel Disease (IBD) includes conditions like leaky gut, Crohn’s Disease, Irritible Bowel Syndrome (IBS) and ulcerative colitis (i.e. ulcers). It can impact joint and gut health and lead to joint inflammation through various mechanisms.
The relationship between IBD and joint inflammation is known as "arthritis associated with inflammatory bowel disease" or "IBD-associated arthritis." Here's are a few ways that IBD can impact joint inflammation:
Immune System Dysregulation
Inflammatory Bowel Disease is characterized by chronic inflammation in the gastrointestinal tract due to an abnormal immune response. This dysregulation of the immune system can also affect other parts of the body, including the joints.
The exact mechanisms by which the immune system is involved in joint inflammation in IBD are not fully understood. However, it is commonly believed that inflammatory mediators and immune cells can travel from the gut to the joints, triggering inflammation.
Systemic Inflammation
IBD is a systemic inflammatory condition, meaning that inflammation can affect various organs and tissues throughout the body - not just the intestines. Systemic inflammation in IBD can cause inflammation by promoting the release of inflammatory cytokines and other mediators that can affect joint tissues and synovial fluid.
Autoimmune Mechanisms
Both IBD and some forms of arthritis, such as ankylosing spondylitis and reactive arthritis, are autoimmune diseases characterized by an abnormal immune response against the body’s own tissues. Shared genetic factors and immune pathways may contribute to the development of both gastrointestinal inflammation and joint inflammation in individuals with IBD.
Types of IBD-associated Arthritis
There are different types of arthritis associated with IBD, including peripheral arthritis, axial arthritis and inflammatory back pain.
Peripheral arthritis affects the peripheral joints such as the knees, ankles, wrists and elbows. It is more common in individuals with ulcerative colitis. Axial arthritis primarily affects the spine and sacroiliac joints and is more common in individuals with Crohn’s Disease.
Inflammatory back pain is characterized by chronic low or lower back pain and stiffness. It can be a precursor to axial arthritis.
Extraintestinal Manifestations
IBD is associated with various intestinal issues such as joint inflammation, skin rashes, eye inflammation, and liver disorders. Joint inflammation in IBD can occur independently of gastrointestinal symptoms and may precede, occur simultaneously with, or follow the diagnosis of IBD.
Management of joint inflammation associated with IBD typically involves treating the underlying gastrointestinal inflammation and controlling joint symptoms.

6. Genetic Factors
Unfortunately, some causes of joint inflammation are effectively out of your control. Genetic factors can play a significant role in predisposing individuals to inflammatory arthritis. Several genes have been identified that contribute to the development of autoimmune and inflammatory joint conditions.
Susceptibility Genes
Certain genetic variations can increase an individual’s susceptibility to autoimmune diseases and inflammatory arthritis.
For example, specific genetic variants within the human leukocyte antigen (HLA) region, particularly the HLA-B27 gene, are strongly associated with the development of conditions such as ankylosing spondylitis, reactive arthritis and psoriatic arthritis.
Similarly, variants in the HLA-DRB1 gene are associated with an increased risk of rheumatoid arthritis.
Immune System Regulation
Genetic factors can influence the regulation and function of the immune system, which plays a central role in the pathogenesis of inflammatory joint diseases. Variations in genes encoding cytokines, chemokines and other immune-related molecules can affect immune responses, inflammation pathways and the balance between tolerance and autoimmunity.
Inherited Autoimmune Disorders
Some inflammatory joint conditions like rheumatoid arthritis, systemic lupus erythematosus and juvenile idiopathic arthritis, have a genetic component and tend to cluster within families. Individuals with a family history of autoimmune diseases or inflammatory arthritis are at an increased risk of developing similar conditions due to shared genetic susceptibility factors.
7. Environmental Factors
Environmental factors can significantly impact joint inflammation and contribute to the development and progression of inflammatory arthritis and other joint conditions. These factors interact with genetic susceptibility and immune dysregulation to influence the onset, severity and course of joint inflammation. Here's how environmental factors can impact joint inflammation:
Infections
Infections, including bacterial, viral and fungal pathogens, can trigger inflammation and arthritis. Certain infections, such as Lyme disease, gonorrhea, and viral hepatitis, are known to cause infectious arthritis by directly infecting the joints or triggering an immune-mediated inflammatory response.
Environmental exposure to infectious agents can increase the risk of developing inflammatory joint diseases in genetically susceptible individuals.
Smoking
Cigarette smoking is a well-established environmental risk factor for the development and progression of several inflammatory joint conditions, including rheumatoid arthritis, axial spondylarthritis and psoriatic arthritis.
Smoking can promote systemic inflammation, activate autoimmune responses and contribute to joint damage as well as disease flare-ups in individuals with existing arthritis.
Obesity
Excess body weight puts added stress on our joints. Extra pounds on our particularly weight-bearing joints - such as the knees, hips, and spine - increase the risk of inflammation and osteoarthritis.
Obesity and high body mass index are associated with an increased risk of osteoarthritis development. Obesity-related factors, such as mechanical stress on the joints, chronic low-grade inflammation and metabolic dysfunction, can contribute to the pathogenesis of osteoarthritis and intensify joint inflammation.
Dietary Factors
Diet plays a role in modulating inflammation and immune responses and may influence the risk of developing inflammatory joint diseases. Certain dietary patterns, such as diets high in saturated fats, refined sugars, and processed foods, may worsen inflammation and contribute to the progression of arthritis.
Conversely, a balanced diet rich in anti-inflammatory foods, such as fruits, vegetables, whole grains, and omega-3 fatty acids, may help mitigate inflammation and support joint health.
Physical Activity and Joint Overuse
Repetitive stress, overuse injuries and mechanical strain on the joints can contribute to joint swelling and degenerative changes, particularly in athletes, manual laborers and individuals engaged in high-impact activities.
Prolonged or excessive physical activity without adequate rest and recovery can increase the risk of developing inflammatory arthritis and exacerbate existing joint symptoms.
Occupational and Environmental Exposures
Occupational hazards, environmental toxins, and exposure to pollutants can contribute to joint inflammation and musculoskeletal disorders.
Certain occupations involving repetitive movements, heavy lifting, vibration or exposure to hazardous chemicals may increase the risk of developing arthritis and joint-related conditions.

8. Psychosocial Factors
Psychological stress, depression and emotional distress can intensify joint inflammation and pain in individuals with inflammatory arthritis and other joint conditions. Stress-induced activation of the hypothalamic-pituitary-adrenal (HPA) axis and release of stress hormones can modulate immune responses and contribute to systemic inflammation. While the exact mechanisms underlying the relationship between psychosocial factors and joint inflammation are complex and not fully understood, several pathways have been proposed:
Neuroendocrine Pathways
Psychological stress activates the body’s stress response systems, including the hypothalamic-pituitary-adrenal (HPA) axis and the sympathetic nervous system, leading to the release of stress hormones such as cortisol and adrenaline. Dysregulation of the HPA axis and prolonged exposure to stress hormones can modulate immune responses, increase inflammation and exacerbate autoimmune and inflammatory processes in the body, including the joints.
Pain Perception and Sensitization
Psychosocial factors can influence pain perception, pain sensitivity and pain processing mechanisms in individuals with joint inflammation. Negative emotions, such as stress, depression and anxiety, can amplify pain perception and increase sensitivity to painful stimuli, leading to greater pain intensity and functional impairment in individuals with inflammatory arthritis.
Health Behaviors
Psychosocial factors can impact health behaviors and lifestyle choices that influence joint health.
Individuals experiencing psychological stress or emotional distress may engage in negative or potentially harmful coping strategies, such as smoking, alcohol consumption, poor dietary habits and physical inactivity.
These choices can lead to joint inflammation, weaken immune function and contribute to the progression of joint disease.
Social Support and Coping Mechanisms
Social support, positive coping mechanisms and effective stress management strategies can mitigate the impact of psychosocial stressors on joint inflammation and improve overall well-being in individuals with inflammatory arthritis.
Strong social networks, emotional support and access to coping resources can buffer the negative effects of stress, reduce anxiety, enhance resilience and promote adaptive responses to chronic illness.
Behavioral Factors
Psychological distress, depression and anxiety may interfere with medication adherence, follow-up care and participation in self-management activities, leading to suboptimal disease management and worse clinical outcomes.
Understanding the interplay between psychosocial factors and joint inflammation is essential for implementing holistic approaches to arthritis care that address the physical, emotional, and social aspects of health.
Joint inflammation can cause pain, stiffness, swelling, warmth and reduced range of motion in the affected joints, impacting mobility and quality of life.
Proper diagnosis, treatment, and management are essential for controlling inflammation, relieving pain, and preserving joint function in individuals with arthritis and related conditions.

Treatment for Joint Inflammation
That’s a lot of information—we know. If you need to take a breather, we understand. After all, we wrote the content.
We’re not sharing this information to scare you or overwhelm you. Our goal is to help everyone who reads this blog stay informed about their health. And, hopefully, be better equipped to advocate for your wellbeing during treatment.
Now that we’ve discussed all the underlying causes and conditions assosciated with inflammation in your body, let’s talk treatment options.
It’s important to note that treatment for joint inflammation depends on the underlying cause, severity of symptoms and individual factors. As with all medical conditions, though, we encourage you to consult with your medical provider before trying to address the issue on your own.
This blog should never replace an open and honest conversation with your medical provider about your physical wellbeing and care needs.
When you consult with your doctor, here are some care strategies to keep in mind:
Medications
Nonsteroidal Anti-Inflammatory Drugs (NSAIDs)
These medications, such as ibuprofen, naproxen and aspirin, help reduce pain and inflammation in the joints. They can be purchased over the counter or prescribed by a doctor.
Corticosteroids
Steroid medications like prednisone can be prescribed to reduce joint inflammation and relieve pain in severe cases. They may be taken orally or injected directly into the affected joint.
Disease-Modifying Antirheumatic Drugs (DMARDs)
DMARDs, such as methotrexate, sulfasalazine and hydroxychloroquine, are used to treat autoimmune forms of arthritis, such as rheumatoid arthritis. They work by suppressing the immune system and reducing inflammation.
Biologic Agents
Biologic drugs target specific components of the immune system to reduce inflammation and slow joint damage in autoimmune arthritis. These agents include tumor necrosis factor (TNF) inhibitors, interleukin inhibitors and Janus kinase (JAK) inhibitors.
Physical & Occupational Therapy
Physical therapy exercises and techniques can help improve joint mobility, strengthen muscles around the joint and reduce pain and stiffness. A physical therapist can develop an individualized exercise program tailored to the person’s specific needs and abilities.
Occupational therapy focuses on improving the ability to perform daily activities and tasks while minimizing stress on the joints. Occupational therapists can recommend assistive devices, ergonomic modifications and adaptive strategies to enhance function and independence.

Lifestyle Modifications
Weight Management
Maintaining a healthy weight can reduce stress on weight-bearing joints and improve joint function. Weight loss may be recommended for individuals who are overweight or obese.
Exercise
Low-impact exercises, such as swimming, cycling and walking, can help improve joint flexibility, strength and range of motion without intensifying inflammation. Regular physical activity can also help reduce stiffness and pain in the joints.
Joint Protection & Tissue Damage Prevention
Avoiding activities that place excessive strain on the joints, using proper body mechanics and practicing joint protection techniques can help prevent further damage and preserve joint function.
Heat and Cold Therapy
Applying heat packs or cold packs to the affected joints can help reduce inflammation, alleviate pain, and improve joint mobility. Heat therapy can relax muscles and increase blood flow. Conversely, cold therapy can numb the area and reduce swelling.
Nutritional Supplements
Some nutritional supplements, like hyaluronic acid, glucosamine, chondroitin sulfate and omega-3 fatty acids, may help reduce joint pain and stiffness in certain individuals. However, evidence supporting their effectiveness is mixed, and it’s important to discuss supplementation with a healthcare provider.
Surgery
In severe cases of joint inflammation and damage, surgery may be necessary to repair or replace an affected joint. Surgical options include arthroscopic surgery, joint fusion, joint replacement (arthroplasty), and more.
Pain Management Techniques
In addition to medication, pain management techniques such as acupuncture, massage therapy, transcutaneous electrical nerve stimulation (TENS) and relaxation techniques could help alleviate joint pain and improve overall well-being.

MHB3® Hyaluronan
If you are looking for a natural way to support your joint health and maintain healthy joints, you should learn more about Baxyl® Joint Support because it contains the gold standard of hyaluronic acids, MHB3® Hyaluronan.
MHB3® Hyaluronan has eight U.S. patents for its proven, all-natural. MHB3 delivers hyaluronic acid (HA) to the synovial fluid in between the joints while also kick-starting the body’s own natural HA production process. It is unique to other hyaluronic acid supplements on the market due to its oral liquid formulation that allows for quick absorption and maximum efficacy. The liquid nature of MHB3 has been proven to be absorbed 3.8x better by the human body than dry or other hyaluronic acid forms. MHB3 holds U.S. Patents are for the prevention and maintenance of osteoarthritis, osteopenia (precursor to osteoporosis), osteophytes (bone spurs) and the amelioration of joint health.
All Baxyl® products are formulated with MHB3 Hyaluronnan. Baxyl’s unique liquid oral hyaluronic acid formula delivers patented and proven ingredients to support and promote joint and bone health. The proprietary ingredient - MHB3 Hyaluronan - is an all-natural, vegan-friendly, non-GMO hyaluronic acid that is bioidentical to the HA naturally produced by the body.
MHB3 Hyaluronan supplements the body with much needed hyaluronic acid while also stimulating your CD44 and RHAMM receptors (which are responsible for natural hyaluronic acid production) in the mouth and throat upon ingestion. MHB3 supplementation creates an HA feedback loop within the body catalyzed by Baxyl’s morning maintenance dose. Customers are encouraged to take Baxyl continually as directed for consistent benefits. Skipping a dose may affect efficacy.
For more research on Baxyl or MHB3, read more about Baxyl’s full line of health supplement products online.

Get your Baxyl Today!
Order Baxyl from the comfort of your own home! Or if you prefer to shop locally and support small businesses, we’ve got you covered. Our products are available at local retail outlet stores, including health markets and chiropractors. Find a retailer here.
Become a Baxyl® Believer
The benefits of Baxyl products are guaranteed by our manufacturer within the first 21 days of use at the recommended dosage or your money back! If you do not feel relief or results within three weeks of supplementation and the suggested dosage, bring back your bottle of Baxyl to the place of purchase (opened or unopened) to receive a full refund from our Customer Service team.
Have any questions? Want to stay up to date on the best methods to relieve knee pain with our regular newsletters? Sign up now!